February 11 is always a day of reflection and remembrance for me. It is trifecta of anniversaries. Perhaps they are all easy to explain individually but what is not easy, is how they are all interconnected. But really, aren’t all things actually interconnected? I always kind of thought they were, but on this day, things started manifesting their connections in ways I never imagined. It is so much to unpack that I won’t go into it all here, but maybe I will someday.
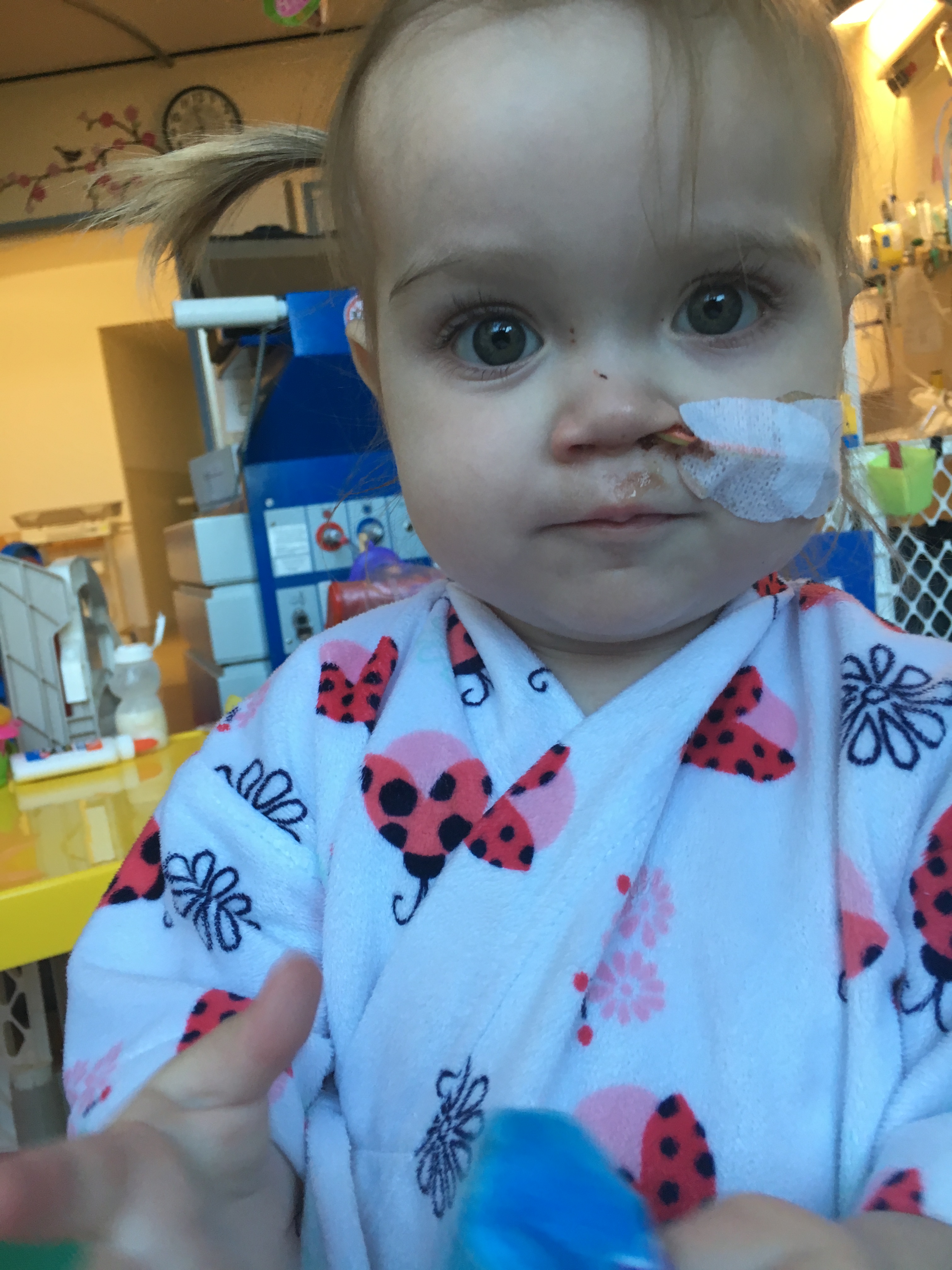
Today is the day, six years ago, I took Hana to the pediatrician at Kaiser. She was five months old and seemed a bit sick with a minor cough and a couple of rounds of vomiting. Her symptoms seemed mild enough but something also seemed really “not right”. My mind and my gut were at odds. “It’s probably nothing and you are a paranoid first-time parent.” is what I thought. “That last time she threw up was not normal. Something really wrong is going on.” is what my gut felt. My mind pretty much always wins but I still got on the phone and had to expedite us getting into the Kaiser system with brand new member numbers (we had just started with Kaiser insurance/healthcare) and then talk to an advice nurse who told me everything was fine. My mind almost hung up that phone and listened to her but my gut pushed me to insist on an appointment with a pediatrician.

A couple of hours later we saw the pediatrician. She ordered a chest x-ray. I remember her voice seemed a little tense. We got the chest x-ray and I remember the x-ray tech looking at me funny after the picture came up. It was very subtle. He was not a radiologist but it was obvious enough, he knew. We walked the five blocks back home. My mind was just doing my normal thing. 40 minutes later the pediatrician called and told us to come back because Hana had an enlarged heart. Her voice was shaking a bit. I didn’t know much but I knew an enlarged heart was not good. We walked back with the stroller. We were greeted by the pediatrician and a pediatric cardiologist and immediately whisked away to an echocardiogram. Hana was calm and cooperative as the echo tech got images of her heart. The pediatric cardiologist was looking over his shoulder the whole time and took over a few times, she seemed anxious.
The cardiologist had us sit in an office and said she would be back. She was gone a while. I didn’t know what to think. Hana was calm and getting tired for her nap. She came back and told us Hana was in heart failure and we were going to go next door to the Emergency Department and wait to be transported to UCSF. I remember being so shocked and confused. I asked stupid questions like, “Would we have to cancel our trip to Hawaii?” (which was in a few days) or “How long would she be in the hospital?” Yes, we had to cancel our trip, she didn’t know how long in the hospital. She knew the severity of what we were likely facing but couldn’t say it, not without more information.
The cardiologist walked us to the Emergency Department. Hana was put in a triage room and hooked up to a monitor. She was calm. There was no cell service in the Emergency Department so when Paul arrived I left to go outside and make some calls. I called my sister to say we weren’t coming to visit her in Hawaii. I called my parents who were about to walk into a birthday dinner for my grandmother.
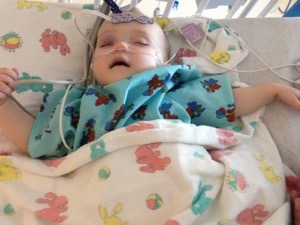
This is how Hana’s heart journey started. She was taken by ambulance to UCSF across town during rush hour. She fell asleep in her carseat and slept the whole time. I started texting friends, Lisa, Chris, Rose, Sue, Kelly. They tried to get an IV started in the CICU and maybe an arterial line? I was bedside when the cardiologist, the head of the pediatric cardiology department at UCSF, called right from there and told her friend she wasn’t going to make it to her birthday dinner tonight. The neonatologist tried to help get things started with the IV or arterial line. No luck. Hana was very fidgety and we read her the same book over and over and over again, it was the only one I had with me. It was late when they gave up and let Hana sleep. The hospital was brand new and had only opened a week before. The staff was still trying to remember the way to the supply closet. Hana tossed and turned all night. I sat by her bedside too afraid to go to sleep because the nurse did not seem to be paying very close attention. I thought one of the IVs they worked so hard to get, was looking precarious but I didn’t know enough then to insist the nurse come and check it. It fell out and when the cardiologist found out the next morning, she was pissed.
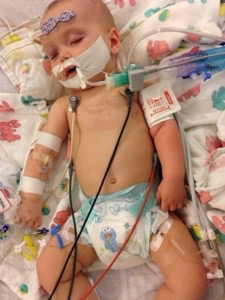
That was February 11, 2015.
I have a previous entry about that day here.
It is also my grandmother’s birthday today, if you picked that up in the story above. I think she would have been 102! As it was, she lived to be 97 and was an amazing woman. I think of her every day. She paid me the greatest compliment I’ve ever been given just days before she died, which was a couple of weeks after Hana was finally allowed to move back home, after nine months of being away, following her heart transplant. Part of me thinks she was waiting for that to happen before departing this earth.

Lastly, and this is the most personal. If you know me, you may not even know this about me. It has to do with God and faith and it is generally something I don’t discuss with people outside of my faith community. Especially in San Francisco where, to have a Christian-based faith, is more often than not, frowned upon and looked at as if you are not very intelligent. This has been my experience. But today is Our Lady of Lourdes feast day. This ties it all together and interconnects it all. It is serendipity at its finest. You can learn more about Lourdes and St. Bernadette from a quick internet search but it is a very special day to people around the world, to Hana and to my grandmother. We went to Lourdes in 2019 and to say it is a special place would not do it justice. For believers and non-believers, it is worth a visit. It has the potential to change your soul, if you will let it.

On another note, I found a piece of paper (see the picture below) – the entry of a yearly calendar for February 11, 2014, when I was pregnant with Hana. I don’t know why I kept the entry for that day, because I didn’t save any other days that year. A few years later, it fell out of a notebook.